The Use of Central Venous Catheters in the Management of Pleural Effusion in a Tertiary Hospital in Cebu City
DOI:
https://doi.org/10.70172/pjcd.v23i1.10295Keywords:
: central venous catheter, pigtail catheter, chest tube thoracostomy, indwelling pleural catheterAbstract
Background: There is limited data on the use of central venous catheters (CVCs) in the drainage of pleural effusions. The study aimed to describe the use of CVCs for this purpose.
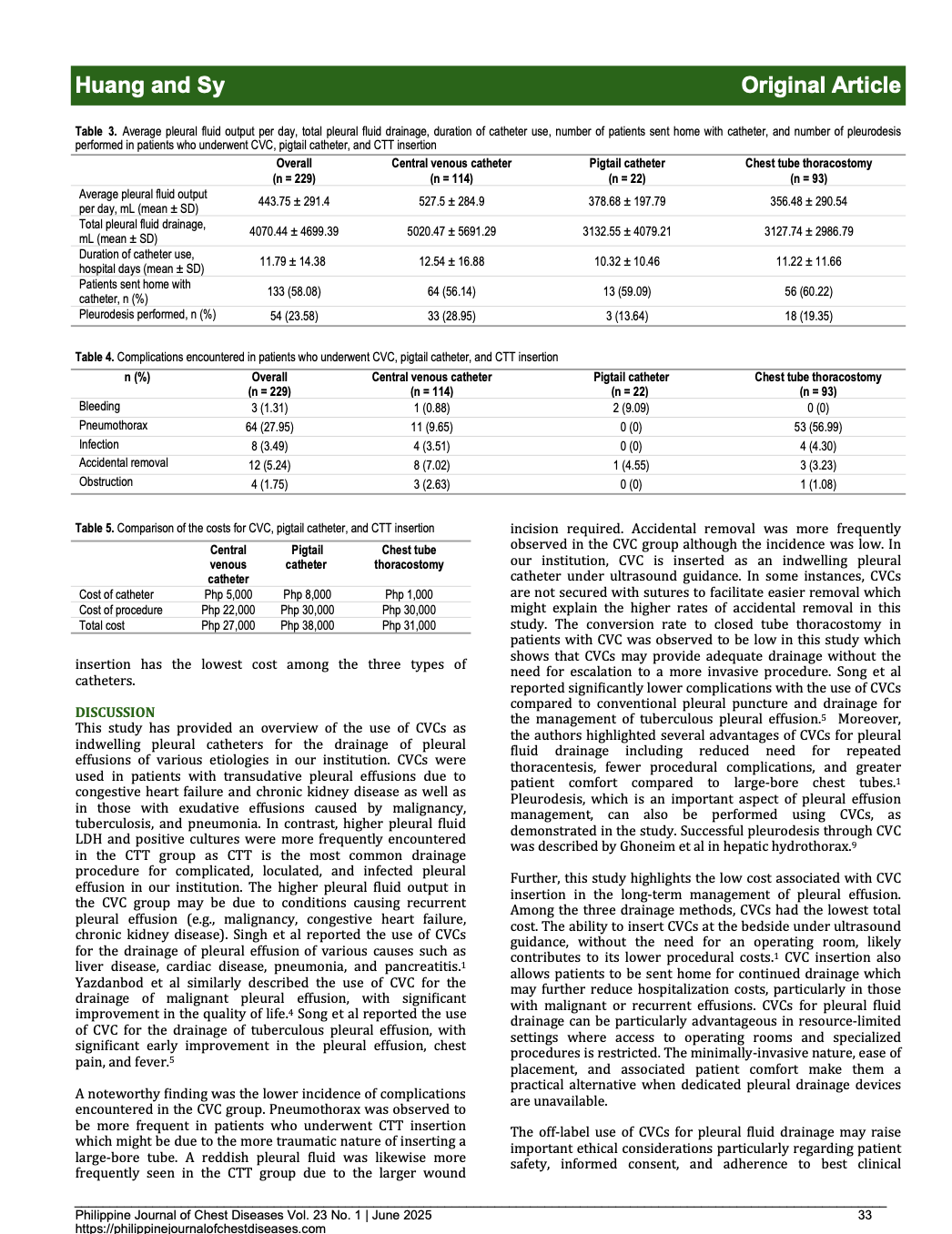
Methodology: This was a cross-sectional descriptive study done in a tertiary hospital in Cebu City. All patients aged >18 years old with pleural effusion who underwent CVC, pigtail catheter, or chest tube thoracostomy (CTT) insertion for pleural fluid drainage were included. Data collected included total drainage of pleural fluid, average daily pleural fluid drainage, duration of catheter use, complications, number of patients sent home with catheters, and number of pleurodesis performed.
Results: A total of 229 patients were included in the study (CVC: 114, pigtail: 22, CTT: 93). Transudative pleural effusion was more frequently encountered in the CVC group (18.78%). Malignancy (28.95%), congestive heart failure (22.81%), tuberculosis (15.79%), pneumonia (15.79%), and chronic kidney disease (14.91%) were the more common causes of pleural effusion in the CVC group. The average daily pleural fluid output and total pleural fluid drainage were highest in the CVC group (527.5 ± 284.9 mL and 5020.47 ± 5691.29 mL, respectively). The duration of catheter use was similar in the three groups. The number of patients sent home with catheters and the number of pleurodesis performed were observed to be highest in the CVC group (48.12% and 61.11%, respectively). Accidental removal was most frequently observed in the CVC group (8/12) although the overall incidence was low at 5.24%. Pneumothorax occurred most frequently in the CTT group (53/64).
Conclusions: The study demonstrates the use of CVCs as an alternative drainage procedure for pleural effusions of various causes. CVCs can also provide an access to perform pleurodesis. A low incidence of complications was observed. Further studies are needed to establish the efficacy and safety of CVCs.
References
Singh, K, Loo, S, Bellomo, R. (2003). Pleural drainage using central venous catheters. Critical Care. 2003;7(6):R191-194. https://doi.org/10.1186/cc2393 DOI: https://doi.org/10.1186/cc2393
Siddiqui, F, Ihle, RE, Siddiqui AH. Intrapleural catheter. In StatPearls. StatPearls Publishing. Accessed May 11, 2025. http://www.ncbi.nlm.nih.gov/books/NBK493229/ DOI: https://doi.org/10.32598/irjns.11.3
Kolikof, J, Peterson, K, Baker, AM. Central venous catheter insertion. In StatPearls. StatPearls Publishing. Accessed May 11, 2025. http://www.ncbi.nlm.nih.gov/books/NBK557798/
Yazdanbod, A, Salehifar A, Maleki, N, Habibzadeh, S, Tavosi, Z. Successful use of central venous catheters in the management of recurrent malignant pleural effusions: One new option. Supportive Care in Cancer. 2015;23(8):2267–2271. https://doi.org/10.1007/s00520-014-2595-3 DOI: https://doi.org/10.1007/s00520-014-2595-3
Song, L, Zhang, Y, Jia, Q. Central venous catheter based closed thoracic drainage in the treatment of tuberculous pleuritis. Pakistan Journal of Medical Sciences. 2019;35(4):1024–1029. https://doi.org/10.12669/pjms.35.4.63 DOI: https://doi.org/10.12669/pjms.35.4.63
Wu, S., Zhang, M. Central venous catheter for coal workers pneumoconiosis complicated with pleural effusion and pneumothorax efficacy analysis. Chinese Journal of Industrial Hygiene and Occupational Diseases. 2015; 33(1): 51-53. https://pubmed.ncbi.nlm.nih.gov/25876977/.
Chest tube insertion (Small bore catheter—CVC) evaluation form. Section of Pulmonary Medicine. Chong Hua Hospital
Cooke, DT and David, EA. Large-bore and small-bore chest tubes: Types, function, and placement. Thoracic Surgery Clinics. 2013;23(1):17–24. https://doi.org/10.1016/j.thorsurg.2012.10.006 DOI: https://doi.org/10.1016/j.thorsurg.2012.10.006
Ghoneim, AHA, El Gammal, MS, AboZaid, MMN, El Rahman, AA. Efficacy of central venous catheter in pleurodesis in refractory hepatic hydrothorax. The Egyptian Journal of Chest Diseases and Tuberculosis. 2019;68(2):236. https://doi.org/10.4103/ejcdt.ejcdt_82_18 DOI: https://doi.org/10.4103/ejcdt.ejcdt_82_18
Downloads
Published
How to Cite
Issue
Section
License
Copyright (c) 2025 Raymond Philip D. Huang, MD, Roger Y. Sy, MD

This work is licensed under a Creative Commons Attribution 4.0 International License.







