Inhaler Technique Comparison Between Dry Powder Inhaler and Metered Dose Inhaler Among Adults with Obstructive Airway Disease in a Tertiary Government Hospital Outpatient Setting
DOI:
https://doi.org/10.70172/pjcd.v23i1.10955Keywords:
inhaler technique, obstructive airway disease, metered dose inhaler, dry powder inhalerAbstract
Background: In the management of obstructive airway diseases, inhaled medication remains a cornerstone of therapy. Aside from medication type, the manner of delivery through various devices is important. Evaluating current practice provides a measure of performance and allows identification of areas for improvement. The study evaluated inhaler techniques of patients on dry powder inhalers (DPI) versus metered dose inhalers (MDI) at the outpatient setting. The prevalence of specific inhaler technique errors was assessed along with associated factors.
Methodology: This study was conducted with a cross-sectional design, involving patients with use of DPI and/or MDI for the past six months. Inhaler technique was evaluated and a short instruction on proper technique was provided with repeat evaluation immediately after.
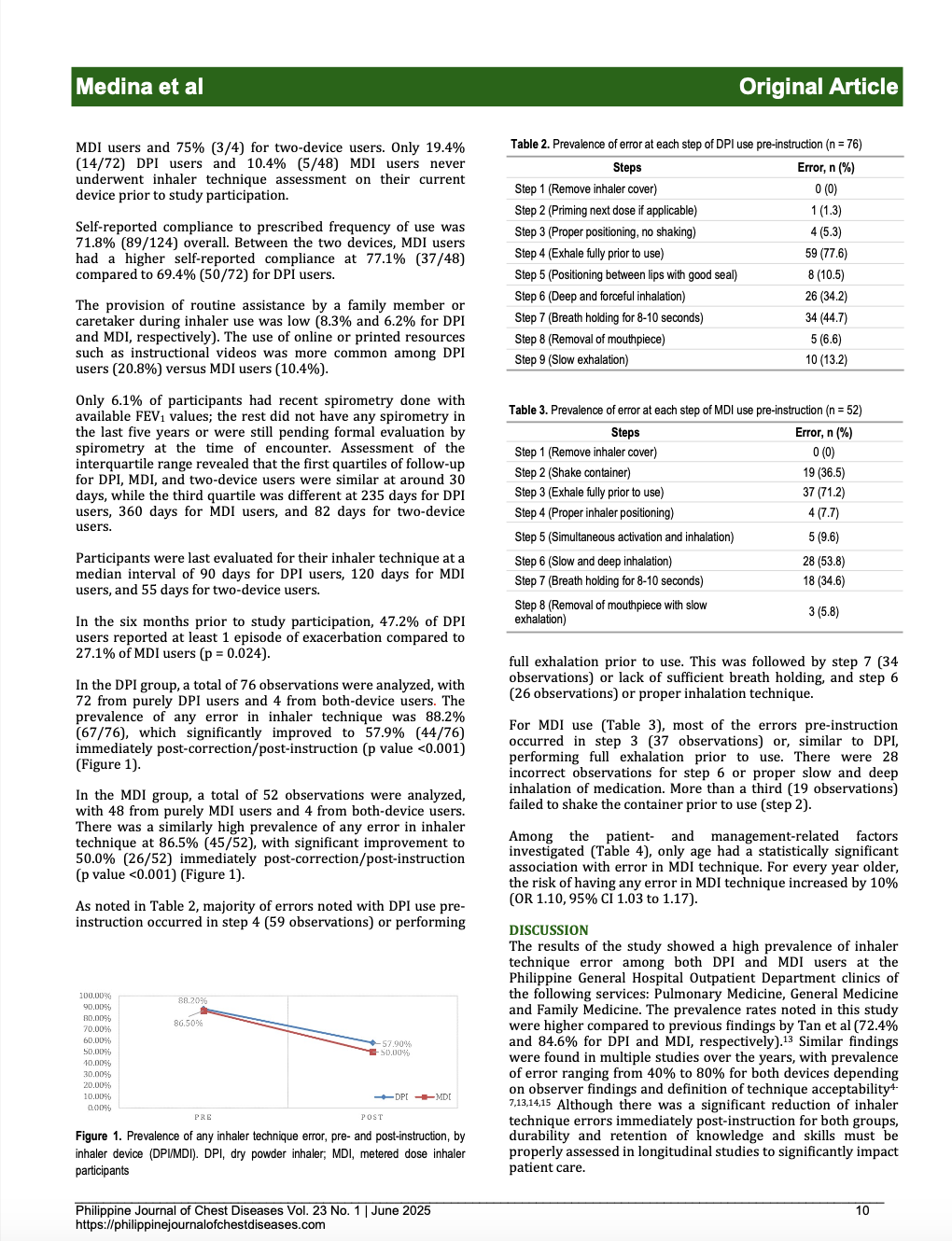
Results: A total of 124 participants were assessed, resulting in 76 DPI and 52 MDI technique observations. Overall, a higher prevalence of any error was observed for DPI at 88.2% versus MDI at 86.5%. Immediately post-instruction, repeat assessment showed significant improvement, with reduction of any error to 57.9% (DPI) and 50% (MDI) (p <0.001 for both). The most common DPI errors were failure to perform full exhalation prior (77.6%) and lack of sufficient breath holding after (44.7%). The most common MDI errors were failure to perform full exhalation prior (71.2%) and improper inhalation (53.8%). For MDI users, only advanced age had an association with having any error (OR 1.10, CI 1.03-1.17).
Conclusion: Inhaler technique errors remain high in the outpatient setting regardless of device, with older participants at risk of having errors with MDI, but not with DPI. Although technique review and instruction show promise in reducing errors, the durability of these skills is known to decay. Appropriate patient and device selection, along with regular technique assessment and reinforcement by healthcare professionals, remains the recommended practice to maximize the benefit of inhalers.
References
Global Initiative for Asthma. Global strategy for asthma management and prevention. 2023. Accessed March 19, 2025. https://ginasthma.org/2023-gina-main-report/
Global Initiative for Chronic Obstructive Lung Disease. Global strategy for prevention, diagnosis and management of COPD: 2023 Report. 2023. Accessed March 19, 2025. https://goldcopd.org/2023-gold-report-2/
The National Asthma Council Australia. Accessed March 19, 2025. https://www.nationalasthma.org.au/living-with-asthma/resources/health-professionals/charts/inhaler-technique-checklists
Fink JB, Rubin BK. Problems with inhaler use: A call for improved clinician and patient education. Respir Care. 2005;50(10):1360-1375. Accessed March 19, 2025. https://pubmed.ncbi.nlm.nih.gov/16185371/
Price D, David-Wang A, Cho SH, et al. Asthma in Asia: Physician perspectives on control, inhaler use and patient communications. Journal of Asthma. 2016;53(7):761-769. https://doi.org/10.3109/02770903.2016.1141951 DOI: https://doi.org/10.3109/02770903.2016.1141951
Lee HY, Song JH, Won HK, et al. Comparing inhaler use technique based on inhaler type in elderly patients with respiratory disease. Tuberculosis & Respiratory Diseases. 2020;84(1):46-54. https://doi.org/10.4046/trd.2020.0021 DOI: https://doi.org/10.4046/trd.2020.0021
Usmani OS, Lavorini F, Marshall J, et al. Critical inhaler errors in asthma and COPD: A systematic review of impact on health outcomes. Respiratory Research. 2018;19(1). https://doi.org/10.1186/s12931-017-0710-y DOI: https://doi.org/10.1186/s12931-017-0710-y
Consumer information: Symbicort Turbuhaler. Consumer information leaflet. AstraZeneca. Accessed March 26, 2025. https://www.astrazeneca.com/content/dam/az-ca/downloads/productinformation/symbicort-turbuhaler-consumer-information-leaflet-en.pdf
Quick guide to using your Symbicort inhaler. Consumer guide. AstraZeneca. Accessed March 26, 2025. https://www.symbicorttouchpoints.com/content/dam/physician-services/us/526-rwd-symbicort-hcp/pdf/03_using_the_symbicort_inhaler.pdf
Seretide Diskus. Product leaflet. GlaxoSmithKline. Accessed March 26, 2025. https://assets.gskstatic.com/pharma/PMPI_portal/Lebanon/seretide_discus_powder_for_inhalation_pil_lb.pdf
Handihaler. Instruction for use. Product leaflet. Boehringer Ingelheim. Accessed March 26, 2025. https://www.manualslib.com/manual/2150937/Boehringer-Ingelheim-Handihaler.html
Ultibro Breezhaler. Information for the user. Package leaflet. Novartis. Accessed March 26, 2025. https://www.medicines.org.uk/emc/files/pil.3496.pdf
Tan, MK, Manua, NP, Roa, CC, Jorge, MC. Assessment of inhalational technique among adult patients with obstructive airway disease at the outpatient department of a tertiary level hospital in the Philippines. Abstract. Philippine Journal of Chest Diseases. 2018;19(1). Accessed March 19, 2025. https://philchest.org.ph/journal/2018/PJCD%20vol%2019%20issue%201_final.pdf
Jolly GP, Mohan A, Guleria R, Poulose R, George J. Evaluation of metered dose inhaler use technique and response to educational training. Indian J Chest Dis Allied Sci. 2015;57(1):17-20. Accessed March 19, 2025. https://pubmed.ncbi.nlm.nih.gov/26410977 DOI: https://doi.org/10.5005/ijcdas-57-1-17
Collier DJ, Wielders P, Van Der Palen J, et al. Critical error frequency and the impact of training with inhalers commonly used for maintenance treatment in chronic obstructive pulmonary disease. International Journal of COPD. 2020;(15):1301-1313. https://doi.org/10.2147/COPD.S224209 DOI: https://doi.org/10.2147/COPD.S224209
Melani AS, Bonavia M, Mastropasqua E, et al. Time required to rectify inhaler errors among experienced subjects with faulty technique. Respiratory Care. 2016;62(4):409-414. https://doi.org/10.4187/respcare.05117 DOI: https://doi.org/10.4187/respcare.05117
Bosnic-Anticevich S, Bender BG, Shuler MT, Hess M, Kocks JWH. Recognizing and tackling inhaler technique decay in asthma and chronic obstructive pulmonary disease (COPD) clinical practice. The Journal of Allergy and Clinical Immunology in Practice. 2023;11(8):2355-2364.e5. https://doi.org/10.1016/j.jaip.2023.04.031 DOI: https://doi.org/10.1016/j.jaip.2023.04.031
Downloads
Published
How to Cite
Issue
Section
License
Copyright (c) 2025 Henry Y. Medina Jr., MD, Ma. Cecilia C. Lozada, MD, Cary Amiel G. Villanueva, MD, Ma. Kriselda Karlene G. Tan, MD

This work is licensed under a Creative Commons Attribution 4.0 International License.







